Part 8: Next-generation COVID-19 vaccines
All COVID-19 vaccines are trying to achieve the same thing – to induce a certain level of immunity to the virus. They do so by stimulating an immune response to an antigen, a molecule found on the virus (Part 5). In the case of COVID-19, the antigen is typically the characteristic spike protein found on the surface of the virus.
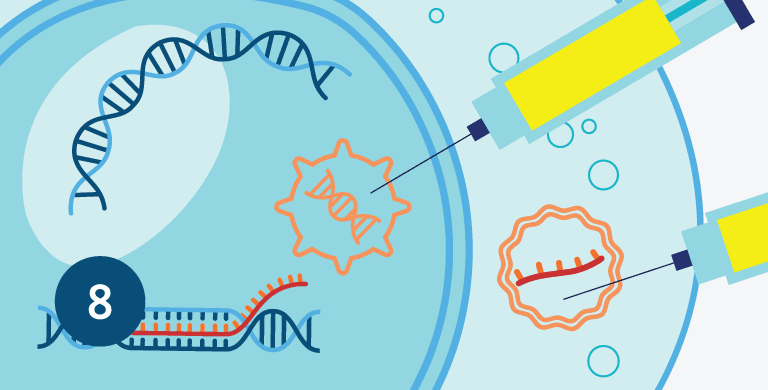
The so-called next-generation vaccines do not contain an antigen, in other words they don’t contain the spike protein itself. Instead, they use the body’s natural capabilities of manufacturing a protein from a DNA or mRNA recipe to teach the body how to recognize the virus.
Some next-generation vaccines use a DNA recipe, while others bypass the first step of protein production (Part 1) and introduce the mRNA copy of the DNA recipe. Both mRNA and DNA are not stable and are quickly broken down in the body. It is for this reason that in both types of vaccines one needs to protect the genetic recipe until it reaches the cell. Once in the cell, mRNA and DNA do not last very long and once they are copied and have produced the protein they code for, their job is done. The body naturally breaks them down together with the clean-up of its own “used” DNA and RNA strands.
mRNA vaccines
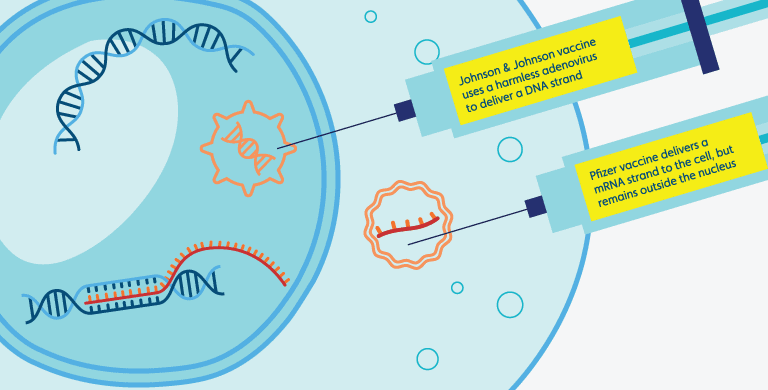
The Pfizer vaccine is a mRNA vaccine and uses a lipid nanoparticle to carry the mRNA to our cells. Once in the cell, the mRNA is read and used to build the virus’ spike protein which the immune system then learns to recognize. There are two very good reasons why mRNA vaccines cannot change your DNA.
Firstly, mRNA cannot be inserted into DNA, as the mRNA would first need to be made into DNA (called reverse-transcription) and humans do not have the enzyme which is needed for this. Secondly, mRNA cannot be transported into the nucleus where our DNA is housed.
Viral-vector vaccines
The Janssen or Johnson & Johnson vaccine is a viral-vector vaccine. Instead of a lipid nanoparticle, it uses a harmless adenovirus to deliver the DNA recipe for the spike protein to our cells. Once there, the DNA is copied into mRNA, and from that point works largely the same as the mRNA vaccine. While this vaccine uses DNA, the type of virus which is used to carry this DNA into our cells does not incorporate it into our own genes, it only uses the ingredients (amino acids) and our cellular machinery to make mRNA copies of the recipe it carries. In fact, scientists previously tried to use adenoviruses to incorporate DNA fragments into human genes as a treatment for Cystic Fibrosis, but this was unsuccessful for two reasons. Firstly, because the virus failed to insert the DNA it carried into the patient’s genes, the beneficial effect to the patient was short-lived, as the body could only use the DNA to produce the functional protein of interest until the DNA was broken down. This would have required repeated doses, but here scientists encountered the second problem. These adenoviruses triggered an immune response, so repeated doses would only train the body to attack and remove the treatment. While these characteristics of adenoviruses made them inappropriate for gene therapy, it qualified them very well for a role in vaccines, where the DNA and its protein should hang around just long enough to train the immune system before disappearing, and where the immune system should be triggered to respond so that it can build up immune memory.